Llansadwrn (Anglesey) Weather
Wx-ScienceWatch
from the observer's perspective

 |
Llansadwrn (Anglesey) WeatherWx-ScienceWatchfrom the observer's perspective |

|
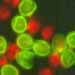
The organism
The illness it causes
Life (cycle) history of Cryptosporidium
How many oocysts are necessary to cause illness
Sources of infection
How is the organism removed and killed?
Can the weather have an effect?
Cryptosporidium and British water supply regulations
Report by the OUTBREAK CONTROL TEAM (28 November 2006)
Welsh Water Dwr Cymru fined as a result of the outbreak (11 October 2007)
Disclaimer: This page is for interest in the science involved and should not be taken as a substitute for seeking medical treatment or any other advice
It is not a virus or a bacterium as some media reports persistently call it, but a protozoan parasite.
Cryptosporidium parvum (C. parvum) is a single celled parasitic organism that lives in the intestinal tract of a wide variety of animals, including farm and wildlife species, and humans. It is a microscopic organism some five thousandths of a millimetre in diameter, less than one-tenth the thickness of a human hair. The protozoan parasite is acquired when people, or animals, ingest contaminated water or food. While the species must have been around, in association with animals for thousands of years, it was not reported as affecting humans until 1976. Although the organism infecting mice, C. muris, was discovered and in 1907 and C.parvum in 1912, both named by Tyzzer, it was overlooked as an important human parasite until 1976. This may have been due to the difficulty of testing for, identifying and culturing the organism in the laboratory; methods have now improved. It first came to prominence through a series of disease outbreaks in the 1980's and 1990's, when it was confirmed as being responsible. Despite meeting all the water standards set at the time in 1987 80% of the population of a town of 16,000 inhabitants in Carrollton, Georgia, U.S.A, became ill. C.parvum was found to be the cause and several other outbreaks, including several Britain, were later confirmed. One of the largest waterborne outbreaks was in Milwaukee, Wisconsin, when in 1993, an estimated 403,000 people became infected following inadequate filtration of the water supply. In Britain in 1999 there was a smaller scale outbreak when an infected sheep contaminated a reservoir supplying Manchester. One of the most recent outbreaks occurred in April 2005 in Perthshire, Scotland, where 200 people reported ill after visiting Auchingarrich Wildlife Centre; on the 22 April there were 32 confirmed cases in visitors since 25 March. There are now about 6000 confirmed cases annually in the UK, but this number is thought to underestimate the total as not everyone would report to their doctor and not all patients would be tested. In 2002 a genotype (I) of C. parvum was recognised as being fairly specific for humans and, although morphologically indistinguishable, has been named Cryptosporidium hominis and is now accepted as responsible for many of the human infections. DNA analyses are now being used increasingly in identification of the genotypes involved and Abrahamsen et al. (2004) have published the complete genome sequence of C. parvum. The team discovered that Cryptosporidium is missing two organelles commonly found in related protozoan parasites. Missing too are several other sequences, related to essential metabolic functions, a possible explanation as to why the organism was difficult to culture in the past. Other groups, working in Virginia in the United states and MRC Cambridge in Britain, have successfully sequenced the genome of C. hominis. It is thought that this work may lead to new strategies, drugs and vaccines for dealing with this important worldwide disease organism.
Infection in Britain seems to affect mostly children under 5 years and young adults. It appears to be less common in babies under 6 months and in adults of 45 years, or more, who seem to show some immunity. In the U.S. It is estimated that between 30 and 45% are immune, whereas up to 65% in less developed countries are immune . But as people become older their immune systems may weaken and they too become vulnerable; there have been outbreaks in care-homes in the past. Also at greater risk are people, of any age, whose immune systems are deficient or suppressed due to drug treatment or HIV-AIDS.
Development of symptoms of this form of gastroenteritis may be slow, incubation may be between 2 and 12 days with a mean of 7 days. It may start with nausea and loss of appetite but later symptoms include sudden onset of diarrhoea, vomiting, stomach cramps and fever. Symptoms are unpleasant, but are self-limiting, and may persist for 1 to 3 weeks in healthy individuals although longer recovery times have been reported. Dehydration can be a problem and those affected are advised to drink plenty of fluids (boiled cooled water) or, better, fluids containing the correct balance of minerals and salts. In severe cases, especially children and seniors, the advice is that medical attention should be sought as soon as possible. There is no effective treatment at present although use of 1 or 2 experimental drugs is being explored.
Life (cycle) history of Cryptosporidium
At least 22 species of Cryptosporidium have been identified having different morphologies and hosts, for example C. felis occurs in cats, C. canis in dogs and C. meleagridis in birds. Perhaps the most commonly found species is C. parvum and was named by Tyzzer in 1907, but what it did in humans remained untold until the latter part of the century it being thought that animals were the only hosts. It is a parasite and needs a host for it's survival, animal or human, to complete it life cycle in 4 phases. (1) Starting outside the body the organism exists as an oocyst, a dormant phase with a tough coat enabling survival for a long time in a harsh environment. It is resistant to disinfectants, including chlorine and can withstand 2 hours in a solution of household bleach, but is susceptible to heat and ultraviolet light (UV) and can be filtered out. When ingested, via water or food, the oocysts in the intestine (phase 2) sporulate (hatch) into 4 sporozoites then they invade epithelial cells of the host's gut. There they undergo a complicated 2 stage (phase 3) asexual reproduction phase followed by a (phase 4) sexual phase in which a new oocyst is produced that is, along with perhaps millions of others, passed back (shed) into the environment in faeces to await ingestion by another host.
How many oocysts are necessary to cause illness?
An interesting question. I have seen estimates that between 10 and 30 are necessary, but there seems to be no hard and fast rule. It is theoretically possible that just 1 organism is perfectly capable of causing illness, certainly less than 10. But It has been put forward by the U.S. Environment Protection Agency that natural, non-specific, immunity is the reason why the infection dose is greater than 1 organism. Thus persons with compromised immune systems are usually susceptible to a smaller number of organisms. The number of organisms required seems therefore to be dependant on the immune status of the host, and this seems likely to vary from person to person.
Sources of infection
Person to person transmission is important as indicated by previous instances of institutional outbreaks. Personal hygiene is important at all times to limit the spread of the organism. Farm and domestic animals can be a source and often show no clinical signs of infection. Cats and dogs have been shown to have infected HIV AIDS sufferers with specific Cryptosporidium genotypes. Food has been identified as a possible source and has included raw fruit and vegetables such as salads and cider, where the apples used were picked up from the ground used as pasture and were contaminated by cattle faeces. Inadequately pasteurised milk has been reported as causing an outbreak at a school. But waterborne organisms appears to be the main source in small and large scale outbreaks to the present day. Swimming pools, properly maintained, do not usually present a risk, but they have been implicated as the cause in a few outbreaks. Personal hygiene of the swimmers is important, showering and washing nude with soap is recommended before swimming. Another possible source is from animal slurries and human sewage deposited on land surfaces. Manuring with farm yard wastes has been done for a long time, but the use of human sewage, with a range of possible pathogenic organisms including the protozoan parasites Cryptosporidium and Giardia and a range of viruses, is new . It is a small but increasing problem as it is regarded as the 'best practicable environmental option' at the moment. The amounts deposited on British soils each year since 1998 are increasing being due to the ban on sea dumping following the European Union Urban Waste Water Treatment Directive 1991 and adopted by the UK in 1994. In 1992 about 470,000 dry tonnes were deposited and by 2005 was expected to double (Warnes & Keevil, 2003).
How is the organism be removed and killed?
Water companies can remove the organism by a process coagulation and filtration. Chemicals are added to the water that causes impurities in the water to aggregate and form large clumps. Filters, usually of sand, can then remove these clumps before the water is chlorinated and distributed. Some domestic filters may remove the organism from water but do not kill it. Therefore the filter substrate remains a concentrated source and extreme care is needed handling and disposing of it. Protocols issued by the manufacturer of the filter must strictly followed through. Heating remains the primary safest method of denaturing (killing) the oocyst and simply cooking food or boiling drinking water to boiling point (100C) is sufficient. It is also killed by the process of pasteurisation in which the liquid (e.g. milk) is heated to 73.3C or 143F usually for 5 seconds, or sometimes longer. Lower temperatures, and heating for longer periods, have been reported as killing the organism. For example composting organic matter at 55C, this takes longer, seems to be effective. Dishwashers are probably safe to use if the temperature setting is high enough and utensils allowed to dry. Desiccation (drying) seems to kill the organism, air drying for 4 hours has been reported to kill the oocysts. Freezing is also effective, but the freezing temperature must be below -20C for several hours.
Can the weather have an effect?
Dry sunny weather with high UV levels can reduce or destroy oocysts in contaminated material on the ground surface., Oocysts are likely to survive, and remain viable for longer, in cloudy and damp weather. Surface water supplies have been known to be infected when heavy rainfall events overwhelm the capacity of sewage systems. There were several heavy rainfall events in northwest Wales in October notably on the 11th with over 50 mm, 18th and 23rd both days with over 30 mm ![]() . Coupled with rising soil water percentages these rains were accompanied by considerable river flow and runoff especially in mountainous areas (it is not unusual for rainfall events in Snowdonia to be 3 to 5 times greater than that recorded on Anglesey). Heavy rains have also washed oocysts from nearby contaminated pasture land leading to infected water supplies. In Cumbria a spring peak in the number of cases of cryptosporidiosis was much reduced after sheep, grazing around Thirlmere in the Lake District (a constructed masonry dam (1890-94) used as a reservoir for Manchester), were removed to other grazings at lambing time. The number of cases in the spring lambing season in north-west England
between 1979 and 2001 was 720 and by 2004 the number, following removal of the sheep had reduced to 182. The spring peak was put down to heavy rain washing contaminated material off grassland into rivers feeding the reservoir. According to a recent study conducted at the Johns Hopkins Bloomberg School of Public Health
in the United States, more than half of the waterborne disease outbreaks in the past 50 years occurred after heavy rainfall.
One of the possible effects of climate change, due to global warming, is to increase the frequency of heavy rainfall events.
. Coupled with rising soil water percentages these rains were accompanied by considerable river flow and runoff especially in mountainous areas (it is not unusual for rainfall events in Snowdonia to be 3 to 5 times greater than that recorded on Anglesey). Heavy rains have also washed oocysts from nearby contaminated pasture land leading to infected water supplies. In Cumbria a spring peak in the number of cases of cryptosporidiosis was much reduced after sheep, grazing around Thirlmere in the Lake District (a constructed masonry dam (1890-94) used as a reservoir for Manchester), were removed to other grazings at lambing time. The number of cases in the spring lambing season in north-west England
between 1979 and 2001 was 720 and by 2004 the number, following removal of the sheep had reduced to 182. The spring peak was put down to heavy rain washing contaminated material off grassland into rivers feeding the reservoir. According to a recent study conducted at the Johns Hopkins Bloomberg School of Public Health
in the United States, more than half of the waterborne disease outbreaks in the past 50 years occurred after heavy rainfall.
One of the possible effects of climate change, due to global warming, is to increase the frequency of heavy rainfall events.
Cryptosporidium and British water supply regulations
The Water Supply (Water Quality) Regulations 1999, designed to deal with Cryptosporidium, came into force in June 1999. The regulations require that water companies carry out risk assessments and, if such a risk is established, must use a process for treating water to ensure that the average number of cryptosporidial oocysts is less than one per 10 L (litres) of water. Water leaving the treatment works must be continuously sampled and analysed daily for oocysts. Water companies take the supply of water very seriously as it is an offence to supply water that contravenes the standard (Hunter 2000). A spokesman for Dwr Cymru Welsh Water said, in an interview on BBC Wales TV on 30 November 2005, that monitoring was being carried out at Llyn Cwellyn 24-hours a day and tests at that time had not shown a problem. Tests and further investigations as to the cause were continuing.
Publication of report by the Outbreak Control Team
A 184 page report by the Outbreak Control Team was issued on 28 November 2006. The cryptosporidiosis outbreak affected 231 people, making it the largest such water borne outbreak in Wales and was linked to the mains water supply from Llyn Cwellyn. No other explanation was identified.
The report states "it would seem likely that one or more people in the catchment area of Llyn Cwellyn had cryptosporidiosis before the main outbreak. Although they would have been ill with diarrhoea, they would probably not have known that this was due to Cryptosporidium. The [organism] "entered Llyn Cwellyn through one or more routes identified from sewage treatment systems in the catchment area. There were no effective barriers to prevent it then reaching the mains water supply". The report says that "The Cwellyn water treatment works appears to have been operated by Dwr Cymru in accordance with regulatory requirements and its risk assessment."
Since the outbreak new ultraviolet treatment that kills the [organism] has been installed. The report concludes that such an outbreak "should not occur again with the proper functioning of the ultraviolet treatment at Llyn Cwellyn." The report has been sent to the Chief Medical Officer for Wales and the Chief Inspector of Drinking Water. It recommends that they should consider the lessons learned from the outbreak and the need for updated guidance about cryptosporidiosis and the water supply.
Welsh Water Dwr Cymru fined as a result of the outbreak
Welsh Water was fined £60,000 on 11 October 2007, with costs of nearly £70,000, after pleading guilty in Caernarfon Magistrates Court to four counts of supplying water unfit for human consumption. Welsh Water, admitted that the company had been slow in implementing, monitoring and sampling its water in 2005. It was said in Court that the managing director of the company and the board of directors were truly devastated and sorry.
The following pages will give further information 1: UPTEN S. J. (2003). Division of Biology, Kansas State University. Basic Biology of Cryptosporidium. Web page.
2: BBC NEWS SCOTLAND (2005). News item: [Perthshire Cryptosporidium] Wildlife bug infection rate rises. Web page. 3: ABRAHAMSEN M. S. (2004) Complete genome sequence of the apicomplexan, Cryptosporidium parvum. Published Online March 25, DOI: 10.1126/ Science1094786. Abstract page. 4: CENTER FOR THE STUDY OF BIOLOGICAL COMPLEXITY. CRYPTOSPORIDIUM WEBSITE for research on the genome, functional genomics and vaccine development. Web page.
5: IRISH AGRICULTURAL & FOOD DEVELOPMENT AUTHORITY (2003). Cryptosporidium parvum in Food and Water Conference Index of Papers. Web page. 6: WARNES S. & KEEVIL C. W. (2003) Survival of Cryptosporidium parvum in faecal wastes and salad crops. Web page.
7: UNITED UTILITIES. Information on the reservoir at Thirlmere, Cumbria. Web page. 8: HUNTER R. F. (2000). Advice on the response from public and environmental health to the detection of cryptosporidial oocysts in treated drinking water. Commun Dis Public Health 3 (1) 24-27. Available on the web: Document in pdf format.
9: DEPARTMENT FOR ENVIRONMENT, FOOD & RURAL AFFAIRS. Preventing Cryptosporidium Getting into Public Drinking Water Supplies. Proposed Policy Solution deals with how monitoring and analyses should be done and the public availability of results. Available on the web: Document. 10: THE OUTBREAK CONTROL TEAM (Anglesey County Council, Anglesey Local Health Board, Centre for Research into Environment and Health, Dwr Cymru, Environment Agency Wales,
Gwynedd County Council, Gwynedd Local Health Board, National Public Health Service for Wales). (2006). Outbreak of cryptosporidiosis in North West Wales, 2005. Press release : Word Document.
These pages are designed and written by Donald Perkins Copyright © 1998 - 2008
Document dated 1 December 2005
http://www.llansadwrn-wx.co.uk